IVF and PGT for Sickle Cell Disease and Family Balancing
Introduction: The Evolution of ART for Sickle Cell
Assisted Reproductive Technology (ART) began after the breakthrough of Patrick Steptoe and Robert Edwards. They achieved the first successful IVF birth in 1978. Since then, knowledge has expanded to include Preimplantation Genetic Testing (PGT).
Nigeria has been at the forefront of adopting these technologies. We established and reported success with PGT for sickle cell carriers. This allows carrier couples to have children free of the disease. Over time, widespread use of this procedure could help eliminate sickle cell disease (SCD).
SCD is a group of disorders affecting hemoglobin, the molecule that carries oxygen in red blood cells. Patients have abnormal hemoglobin S, which distorts red blood cells into a sickle shape. This article explains the role of IVF and PGT in managing SCD.
The Link Between IVF and Sickle Cell Disease
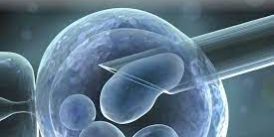
In vitro fertilization (IVF) is an assisted reproductive technique. Doctors retrieve eggs from the female and collect sperm from the male. They then combine them manually in a laboratory dish.
Since 1978, IVF procedures have advanced. Newer techniques like Intracytoplasmic Sperm Injection (ICSI) and PGT have emerged. These advances allow us to assess embryo viability and genetics. PGT serves as both a preventive and corrective procedure for genetic diseases like SCD.
According to the WHO, sickle cell disease is the most prevalent genetic disease in Africa. About 75% of patients live in sub-Saharan Africa. Nigeria alone records over 100,000 new cases each year, making it a critical African health issue.
Nigeria celebrated its first IVF success in 1989, thanks to Prof. Oladapo Ashiru and Prof. Osato Giwa-Osagie at Lagos University Teaching Hospital. This milestone was the first in Sub-Saharan Africa. Since then, awareness and the number of fertility clinics have grown significantly. The next step was establishing advanced technologies like PGT.
A Brief History of Assisted Reproductive Technology
The history of ART dates to 1969, with reports on sperm capacitation in hamsters. This process is essential for fertilization. In 1977, researchers Andrew Schally and Roger Guillemin won the Nobel Prize for isolating LHRH from the hypothalamus. In 1978, Ashiru and Blake reported the FSH positive feedback mechanism on the pituitary.
These discoveries paved the way for the first “test-tube” baby, Louise Brown, in 1978. Robert Edwards later received the Nobel Prize for this achievement in 2010.
Other countries soon followed with their own successes:
-
Australia (1980)
-
USA (1982)
-
Nigeria (1984, with the first delivery in 1989)
What is In Vitro Fertilization (IVF)?
IVF achieves fertilization outside the body. The process involves several key steps:
-
Ovulation induction
-
Oocyte (egg) retrieval
-
Sperm preparation
-
Insemination and fertilization in a culture dish
-
Embryo transfer
Doctors perform egg retrieval and embryo transfer under ultrasound guidance. They handle sperm and eggs under strict temperature control. Without IVF, Preimplantation Genetic Diagnosis (PGD) would not be possible.
What is Preimplantation Genetic Diagnosis (PGD)?
PGD tests for specific genetic defects in an embryo’s DNA before implantation. It targets known genetic abnormalities in the couple. Doctors first performed PGD in the early 1990s to help couples avoid passing on genetic diseases.
At Medical Art Center, we offer PGD for conditions like sickle cell anemia and chromosomal disorders. We collaborate with Genesis Genetics, a world-renowned genetics institute.
Does PGD Replace Prenatal Testing?
No, PGD does not replace tests like chorionic villus sampling (CVS) or amniocentesis. PGD is a pre-pregnancy, research-based test. Prenatal testing remains the gold standard in modern obstetrics and is still recommended if a pregnancy occurs.
The History and Indications for PGD
Researchers performed the first embryo biopsy on rabbits in 1968. In humans, UK scientists developed PGD in the mid-1980s as an alternative to prenatal diagnosis. Initially, it determined gender to avoid X-linked disorders. The first unaffected child after PGD for an X-linked disorder was born in London in 1989.
PGD grew popular in the 1990s for severe disorders like sickle-cell anemia. In 2013, our team published the first success in Nigeria using PGD to deliver a sickle cell-free baby boy. As of 2006, clinics have reported over 15,000 PGD cycles. It is now available for most known genetic mutations.
Common Reasons for PGD Include:
-
Autosomal Dominant Disorders: One partner carries a defect (e.g., Huntington’s Disease).
-
Autosomal Recessive Disorders: Both partners are carriers (e.g., Sickle Cell Disease).
-
X-linked Disorders: One partner carries an X-linked defect (e.g., hemophilia).
-
Chromosomal Abnormalities: One partner carries a structural issue (translocation, inversion).
-
HLA Matching: To select an embryo that is a human leukocyte antigen (HLA) match for a sibling needing a bone marrow transplant.
Understanding Sickle Cell Anemia
Sickle cell anemia is a hereditary condition. A mutated form of hemoglobin distorts red blood cells into a crescent shape. The disease causes severe pain, infections, and an increased risk of death.
In Africa, the highest prevalence of the sickle-cell trait occurs between 10% and 40% of the population in some regions. In parts of Uganda, it is as high as 45%. The geographic distribution of the trait closely matches that of malaria.
PGT can distinguish between genetically normal or affected embryos. It is the only way to determine an embryo’s genetic condition before pregnancy.
The Step-by-Step PGT Process for Sickle Cell
1. Preliminary Probe Preparation (8-10 weeks)
Before PGT, the lab must create a specific genetic probe. This requires DNA samples from direct family members (parents or siblings of the couple). The probe tests the biopsied embryo cells.
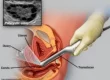
2. Oocyte (Egg) Retrieval
The female partner receives medication to stimulate multiple egg development. A doctor then retrieves the eggs using a unique ultrasound-guided technique under sedation. The eggs rest in an incubator before fertilization.
3. Fertilization via IVF or ICSI
For PGT, fertilization often uses Intracytoplasmic Sperm Injection (ICSI). Under a specialized microscope, a single sperm is injected directly into an egg. This ensures high fertilization rates. The embryos then develop in the incubator.
4. Embryo Biopsy (Trophectoderm Technique)
We perform the biopsy at the blastocyst stage (Day 5 or 6). The embryo then has about 100 cells. Using laser technology, we remove 4-5 cells from the outer layer (trophectoderm), which will form the placenta. This method is less traumatic than older techniques. After biopsy, we immediately freeze all embryos.
5. Embryo Cryopreservation (Freezing)
We preserve biopsied embryos using a rapid-freezing technique called vitrification. We store them in labeled devices within liquid nitrogen tanks, where they remain safely for years.
6. Genetic Analysis in the Lab
The biopsied cells undergo Polymerase Chain Reaction (PCR) to amplify the DNA. Technicians then analyze the DNA to identify the sickle cell status (HbAA, HbAS, or HbSS). We receive results from our collaborating lab within about five days.
7. Embryo Transfer
We prepare the patient’s uterine lining with medications. Once ready, we thaw the genetically normal (HbAA) embryo(s). Using ultrasound guidance, we transfer one or two embryos into the uterine cavity. A pregnancy test follows two weeks later.
Results and Discussion
Today, sickle cell carrier couples in Nigeria can screen their embryos to have a disease-free child. Our clinic has helped many couples achieve this.
While the cost is significant, it offsets a lifetime of medical expenses and stress associated with sickle cell disease. We hope governments and organizations will help make this technique more accessible.
Finally, research continues to improve the speed and reduce the cost of diagnosis. Our experience also shows that environmental toxins and diet significantly impact fertility and IVF success. Therefore, comprehensive detoxification programs, like Mayr therapy, can enhance outcomes by removing heavy metals and allergens from the body.
Acknowledgement: We acknowledge the dedicated efforts of our past and present medical team at the Medical Art Center.